
The Health Information and Management Systems Society (HIMSS), a global non-profit focused on promoting better health through information technology (IT), defines interoperability in healthcare as:
With the advent of value based and coordinated care, and their emphasis on provider collaboration across the care continuum, today’s health systems, physicians and other providers are on a path to implement solutions to enable the exchange of health information. While historically regulatory mandates such as Meaningful Use may have encouraged providers to simply mark “achieve interoperability” off the to-do list and move on to the next chore, advanced functions such as population health management (PHM) require a different, on-going approach to interoperability. Rather than being a once and done endeavor, provider organizations must constantly monitor and update IT models, systems, platforms and infrastructure to enable the best possible, ongoing exchange of data.
The increased demand for information exchange and interoperability enabling solutions has resulted in a market explosion of vendor offerings. While this variety makes for an exciting time in healthcare technology, there has yet to emerge a “golden standard” interoperability solution that has demonstrated the ability to fit the multitude of potential scenarios spanning today’s complex healthcare industry. The market is filled with an array of interoperability possibilities, including public and private HIEs, population health management software, analytics platforms and the ever present EHRs. Each option presents its own set of opportunities, challenges, costs and capabilities. Decoding the offering of these existing solutions can be a challenge on its own. Even more challenging is to determine how one’s organizational needs ultimately align with each solution offering.
To outline a high level approach to the challenge described above, ECG has developed a framework and approach to assist providers in identifying an appropriate interoperability solution.
ALIGNMENT OF ORGANIZATIONAL NEEDS WITH THE RIGHT SOLUTION IS CRITICAL
Provider organizations cannot rely solely on the software vendor market to guide them in selecting an appropriate interoperability solution that may not reflect internal needs and strategies. There must be a thorough analysis that includes an organizational assessment—focusing on the depth and breadth of data exchange needs, both current and future, and the appropriate alignment with existing vendor solutions.
Below is a high-level approach to guide providers in identifying what may be the appropriate solution based on their interoperability depth and breadth requirements.
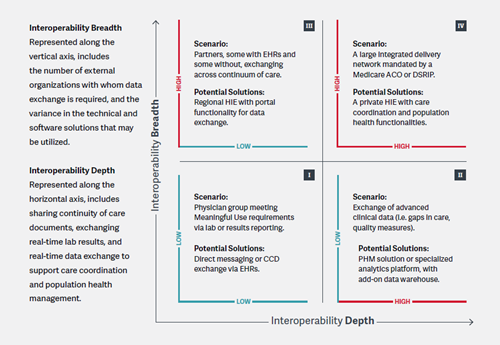
Below are four different interoperability scenarios and potential solutions, ranging across the parameters described above.
Quadrant I: LOW Interoperability Depth and LOW Interoperability Breadth
| Scenario: A physician group is trying to meet the transitions of care requirements of Meaningful Use. This requires the exchange of continuity of care documents, or lab results, with partners capable of receiving secure direct messages through their EHRs. | Solution: Functionality embedded within an organizational EHR, such as direct messaging and the ability to submit continuity of care documents, may suffice. |
Quadrant II:LOW Interoperability Depth and HIGH Interoperability Breadth
| Scenario: A regional safety net hospital system has a large number of partners across the continuum of care including acute hospitals, specialty clinics, community based organizations—some with EHRs and some without. | Solution: Relying on EHR based functionality will likely not be sufficient, given the large variety of technical solutions across the partners. Enabling connectivity through a regional health information organization may suffice, including portal functionality that allows partners lacking an EHR solution to view and submit required information. |
Quadrant III:High Interoperability Depth and Low Interoperability Breadth
| Scenario: A specialty surgery center with a research arm that requires advanced data analytics, such as identifying gaps in care, apply risk-segmentation across a population of patients, or collecting quality measures across the continuum of care to support at-risk payments. | Solution: Functional depth can be provided by population health management (PHM) vendors, or specialized analytics platforms. In an environment of low partner complexity, such solutions may suffice on their own, in most cases along-side a dedicated enterprise data warehouse. |
Quadrant IV: High Interoperability Depth and High Interoperability Breadth
| Scenario: A large integrated delivery network engaged in at-risk payments mandated by programs such as a Medicare ACO or Delivery System Redesign Incentive Payment (DSRIP). Challenges can include complex care coordination, advanced analytics and population management, as well as a large community of technologically diverse partners. | Solution: Existing stand-alone PHM platforms historically struggle to support connectivity across a large and complex population of partners. A comprehensive strategy and solution toolset may be required. |
Case Study
Given the plethora of options available for data exchange and enablement of interoperability, the selection of the right solution is not an easy task. Yet, it is a necessary task, since choosing the wrong solution—one not aligned with the organization’s set of needs—can be costly. A west coast based regional hospital had founded a local health information exchange back in 2010. While the HIE provided a relatively wide set of capabilities, including DIRECT messaging, a patient portal, communication of lab results and community-wide analytics, it was not extensively utilized. Despite an investment of close to $1.5M annually, participating providers made use mostly of the DIRECT function to enable the sharing of continuity of care documents. As the organization and other members of the HIE’s community began moving gradually to more advanced EHR platforms, ECG assisted the regional hospital to conduct an assessment of its interoperability needs against the capabilities that can be provided through its new EHR platform, and the capabilities provided through its HIE. The assessment resulted in a realization that the organizations needs could be mostly met through EHR based connectivity, invalidating the need for continued support of the HIE and achieving considerable savings.
CONCLUSION
While the vendor landscape continues to evolve and morph, the need for a strategy for organizational alignment with interoperability solutions remains a permanent constant. Even though the danger of misalignment between one’s needs and the solutions selected is real and can be costly, the benefits of alignment are real as well. Data-centric healthcare, enabled through interoperability and information exchange is the backbone of value based care — When implemented properly and in a cost-effective way it benefits providers and patients alike.

