
Healthcare organizations can no longer question whether vertical and horizontal integration are vital to their success; their future viability depends on it. Since withstanding challenges to its legitimacy, the Affordable Care Act (ACA) has catalyzed rapid transformation of the fee-for-service payment model across the healthcare industry. Specifically, transformation efforts have focused on shifting financial risk to providers and incentivizing value-based care (high quality and low cost). During the past year, for example, numerous announcements from the likes of the Department of Health & Human Services (HHS) and the Health Care Transformation Task Force have outlined intentions to shift significant portions of reimbursement to alternative, risk-based payment models within the next 3 to 5 years.1
To flourish in this dynamic environment,providers need to demonstrate the ability to reliably deliver high-value care. Doing so, however, requires strategic, financial, and clinical integration across a full continuum of healthcare services. Many healthcare organizations are facing an intensifying strategic need to undertake rapid growth and assimilation initiatives during the coming years in order to develop a comprehensive portfolio of integrated clinical services. For organizations that do not currently possess the complete suite of services they want or need to be competitive, the question is “Do we build, buy, or align with existing organizations in order to provide missing services?”

The most successful organizations are proactively assessing their clinical capabilities and quickly filling existing holes with the appropriate programs and services. They begin by examining their current continuum of services and answering the following questions:
- What services are necessary for our clinical portfolio and enable us to successfully compete ina value-based environment?
- What is the relative priority of these services?
- How quickly do we need to fill these gaps in our service offerings?
Given the pace of change, acquisition (versus organic growth) will be the optimal strategy for many organizations with service gaps to fill. This article explores the question of whether to build, buy, or align and provides a framework for healthcare leaders to formulate an approach to developing a clinically integrated network in a rapid manner.
THE CASE FOR CLINICAL INTEGRATION
In the value-based payment environment, two issues will drive organizations’ priorities for service integration: (1) the ability to attract and maintain patients and (2) the ability to control costs.
To attract and maintain patients, organizations need a robust, tightly integrated, and high-performing primary care network. Primary care continues to serve as an entry point into the health system; in addition, primary care providers are playing an increasing part in the health management of the network’s patients. Demand for primary care services is surging as more individuals are covered by health plans, the population continues to grow, and the role of primary care providers expands.
An integrated primary care network and tight alignment with select subspecialists are prerequisites for controlling the cost of care. Unlike their role as “gatekeepers” in the 1990s, primary care providers’ responsibilities will now include directing patients to providers/services with a demonstrated track record of delivering high-value care. If the primary care network is not aligned with the health system, there is a greater risk that patients will be directed outside of the health system; or perhaps more harmfully, unaligned primary care providers may be ambivalent about or even have divergent incentives from the health system regarding the cost of care provided to patients.
At the same time, it will be critical to closely align with providers that have historically driven considerable expense in the healthcare industry. This is especially true in areas where there may be a range of therapeutic options with varying impact on the total cost of care. Of particular interest will be services related to typically high-cost clinical programs such as cancer and the cardiovascular and musculoskeletal systems.

Swedish Medical Center (SMC), based in Seattle, Washington, is one health system that recently recognized and proactively responded to the opportunity to tightly align primary care providers to control costs. The health system employed nearly 150 primary care physicians through Swedish Medical Group and had a strong affiliation with Minor & James Medical, which included governance and financial support without full ownership. Minor & James Medical was a multispecialty group with approximately 30 primary care providers. In 2014, SMC executed a strategic relationship with Pacific Medical Centers (PacMed), a primary and specialty care physician organization with more than 60 primary care physicians. SMC entered into a member substitution model in which it replaced PacMed’s sole corporate member. The stated goal of the affiliation was to reduce costs for all stakeholders while improving patient outcomes. PacMed expressed the need for a larger corporate partner to support its ongoing cost-reduction efforts, helping it to achieve economies that it could not achieve on its own. For its part, SMC acknowledged PacMed’s track record of providing low-cost, high-quality coordinated care and expressed a desire to be able to replicate learnings from PacMed across the SMC network.
IDENTIFYING GAPS IN THE SERVICE PORTFOLIO
As organizations seek to forge an integrated, high-value network, an assessment of current resources and clinical capabilities is necessary. Specifically, a gap assessment helps identify the clinical capabilities and resources the organization currently possesses and compares those to the capabilities it will need to be successful in the near and mid terms. It is likely that for many organizations, critical services in the near, mid, and long terms will include:
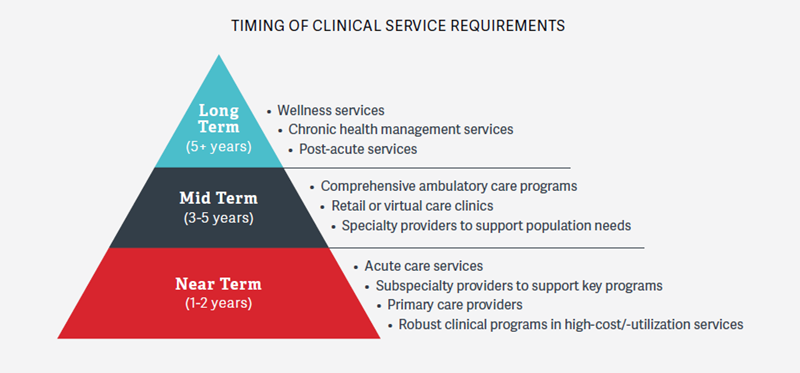
In evaluating and prioritizing missing services, there are a number of key variables to consider, including:
- The financial impact on the organization (from both near- and longer-term perspectives) ifthe service is or is not controlled.
- The strategic importance of the service for building or maintaining program volumes.
- The current organization of the service—does it exist in the community, is it consolidated orfragmented, and are current providers of the service aligned with the health system?
- The relative strength or performance of current service providers.
- Trends indicating that health plans are likely to accelerate financial risk associated with therelated clinical program.
- Other political and stakeholder considerations that may support or conflict with these priorities.
PROJECTED TIMING OF MARKET DEMANDS
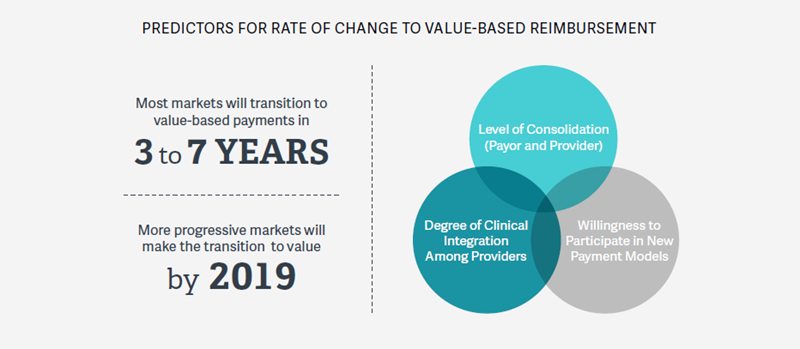
Once critically needed services are identified, an organization needs to assess how quickly the reimbursement environment will transition to value-based payments. This timing dictates the pace at which the organization needs to incorporate these services. However, based on available information, most markets will likely shift significant portions of reimbursement to value-based payments within 3 to 7 years.
Within this time frame, the pace of transition to value-based payments will vary by market. A more specific timeline of change for a given market can be predicted by examining the regional payer and provider landscape. In particular, a market’s readiness for value-based payments can be predicted by:
- The level of consolidation among market players.
- The organizations’ historical willingness to develop or participate in different reimbursement models.
- The level of clinical integration among healthcare providers in the market.
The rate of payment innovation, in most markets, will be determined by governmental payers, as commercial health plans often follow CMS’s lead. CMS has announced plans to require a substantial portion (50%) of its payment to be dependent upon performance within the next 3 years. How commercial health plans keep pace with this change can usually be projected by a health plan’s historical level of innovation (e.g., more innovative plans are likely to adopt value-based payment models at a faster pace). The market share of the payer can also be a good indicator. Larger, more dominant payers are expected to move to value-based payments more rapidly than smaller plans due to their ability to manage new payment models and drive change in the market. In more progressive markets, assuming that commercial plans match Medicare’s pace of payment innovation, health systems could see many of their commercial plans incorporate value-based payment metrics by 2019.
The other key consideration is the degree of integration and consolidation among healthcare providers in the market. Markets with significant provider integration and consolidation are often more responsive. Consolidated providers generally are better equipped to adapt to changing health plan efforts; therefore, it is probable that value-based reimbursement will progress more rapidly in these markets. Likewise, health plans are more likely to pilot new reimbursement models in markets with health systems that have historically shown an aptitude for and interest in alternative reimbursement models.
BUILD, BUY, OR ALIGN?
So, what do organizations with identified needs for particular services do? Do they build (develop) or buy (acquire) these services, or do they align themselves with another organization that offers the needed set of services?
Build (or develop) – The “build” option focuses on developing a de novo clinical service. Typically, this necessitates bringing new providers into the community and assembling other requisite infrastructure, such as clinic space, as well as associated diagnostic or therapeutic capabilities. Moreover, this strategy requires organizations
to develop institutional knowledge and expertise to manage the operations of the program and strategically position it for success. Typically, this will be accomplished by hiring seasoned leaders (administrative and/or clinical) for the program. The success of the program is dependent on its ability to either service unmet demand in the market or to change care-seeking patterns. While this is often the slowest approach to program development, it offers the opportunity to customize the program to meet the needs of the health system without contending with established systems, processes, or personnel.
Buy (or acquire) – The “buy” approach to program development seeks to acquire and utilize existing infrastructure (providers, technology, administrative leadership, etc.). Utilizing existing clinical infrastructure can simplify program development by minimizing the need to assemble new resources, as in the build approach. Thus, program development through acquisition is usually an efficient and expedient
strategy. Also, acquisitions are typically advantaged by the presence of an established client base (patient panels or referral relationships), which minimizes the need for ongoing investments to develop the program.
Align – The alignment approach is often utilized when there is an established provider or program in the market that the health system would like to incorporate into its continuum of care, but for a variety of reasons, the provider/program is unwilling or unable to be acquired by the health system. In these circumstances, the alignment model may serve as a “next best” option to acquisition, as it capitalizes on existing infrastructure. Generally, organizations will realize the greatest level of alignment benefit when there are congruent financial incentives and shared decision making between the parties. Traditional models that achieve significant alignment have included professional services agreements, comanagement agreements, and joint ventures, among others. In recent years, organizations have also used managed care strategies such as medical homes, ACOs, and clinically integrated networks to achieve alignment. These and other related models will likely continue to be popular options among physicians and health systems as alternatives to acquisition models.

Each of these options presents potential strategic advantages to program development and integration. The ideal strategy will vary by organization and clinical program. In order to identify the optimal approach, organizations need to carefully assess the pros and cons, while at the same time weighting these considerations in order of importance to the organization.

There are a number of considerations that organizations should evaluate in selecting their clinical program integration strategy (presented to the right). For instance, if your health system determines that it needs an orthopedic surgery practice and existing service providers can be effectively integrated into the health system’s operations, the organization should strongly consider a buy approach. In many cases, it will not be necessary to evaluate all eight considerations, as one or two may be most critical to the organization. However, the additional considerations may be useful in determining how best to proceed in more complex situations.
Evaluating these considerations will help organizations determine the preferred strategy to internalize the needed clinical capabilities they have identified. Still, in certain cases there may be other considerations that supersede those presented here. In particular, timing may trump a number of other considerations. As markets begin to shift to value-based payment models, organizations will likely find that internalizing certain clinical services in a timely manner is a strategic and/or financial imperative for the organization. In such cases, acquisitions are likely to be the preferred approach to clinical integration.
ACQUISITIONS: THE NEW NORMAL
The pace of change in the healthcare market and the need for healthcare organizations to quickly forge integrated delivery systems will have a significant impact on selection of the preferred clinical integration strategy. As mentioned, the acquisition approach is advantaged vis-à-vis the other models, given the speed with which it can be executed while still achieving the organization’s needs for clinical and financial integration.
As time passes and the industry moves along the continuum to value-based payments, the imperative for clinical integration will continue to grow, yet the time available to enact such integration in a manner that meets the organization’s needs will decrease, thus increasing the reliance on an acquisition strategy. Similarly, given competitive dynamics between organizations, in many instances there is likely to be more than one organization vying to develop or acquire specific services. In these cases, the ability to move quickly (acquire) will be a competitive advantage. Thus, success in a value-based payment environment is dependent in part on organizations developing the capabilities (people, processes, etc.) to quickly identify, prioritize, and assimilate other healthcare provider organizations. Now is the time to assemble the requisite infrastructure to successfully drive regional integration.
Footnotes
1. In January 2015, the Health Care Transformation Task Force, composed of payers and providers, was formed and articulated a goal of shifting 75% of its members’ business payment models into arrangements that incentivize quality and lower-cost healthcare. That same month, HHS announced “a goal of tying 30% of traditional, or fee-for-service, Medicare payments to quality or value through alternative payment models, such as Accountable Care Organizations (ACOs) or bundled payment arrangements by the end of 2016, and tying 50%of payments to these models by the end of 2018.”

