
General Hospital is facing several challenges: declining reimbursement, increasing regulatory pressures, rising operating expenses, growing capital demands related to information technology (IT) and facility upgrades, and paltry investment income. Despite these pressing problems, leadership is devoting the largest share of time and concern to how to proceed with its physician strategy. Like many hospitals, General Hospital has been employing physicians at an increasing rate, both primary care and specialist. This strategy has largely been reactionary. Local physicians are increasingly approaching hospital leadership looking for an alternative practice arrangement, often citing employment offers from other hospitals. Couple this with new physicians seeking a stable practice setting with robust infrastructure, and General Hospital is facing physician network growth that was not part of the long-term plan. This growth is leading to fatigue among leadership – fatigue from negotiating and managing practice acquisitions, from on-boarding physicians, and from having to manage the growing financial losses stemming from the hospital’s expanding physician network.
The situation facing General Hospital is an increasingly common one for hospitals and health systems across the country. Hospital and health system leadership is confronted with a complex set of dynamics that need to be fully understood by the stakeholders and reflected in strategic and operational decision making. At the core, your organization needs to focus on two fundamental issues:
- Strategic Rationale – Identifying the strategic drivers of an employed physician network in your market, and understanding how the physician network is critical to broader organizational strategy.
- Management Evolution – Determining the financial and operational characteristics of the physician enterprise, and being willing to design and manage the network accordingly.
Strategic Drivers
The drivers of physician employment vary by organization, but they generally include at least two of the following:
- Community Need – Hiring physicians can be the most effective way to attract providers and thereby meet patient access needs.
- Market Share – Maintaining/protecting market share often leads to employing physicians who may otherwise close their practices or become employed by a competing organization.
- Service Expansion – Expanding the range of services within the community is often achieved by employing physicians with expertise not currently available in the market.
- Population Management – Employing physicians is often the most direct way to build a coordinated delivery network in fragmented markets.
The Employment Imperative
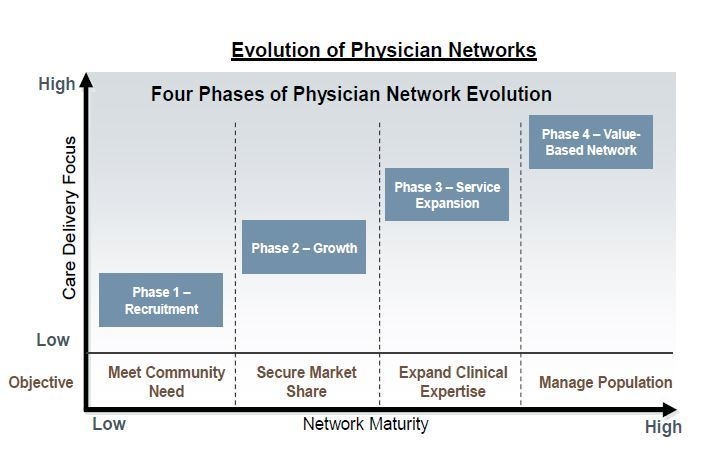
Most organizations fall somewhere on the continuum shown in the figure on the right as their physician network strategies evolve from a recruitment to a delivery focus. Regardless of where you are within this evolution, the reality is that your competitive environment and payer requirements will together determine the pace of the integration process.Whether it involves PCPs or specialists, you cannot let your admitters be recruited by your competitors, you must respond to the migration of Medicare and private payers to value-based reimbursement, and you must bring needed providers and services to the community. If you are the only hospital in the area, you can deliberate on the various aspects of employing physicians. Otherwise, the demands of the providers, community, and payers mean that physician employment, or employment-like arrangements, is your best bet for success and must be an integral part of your strategy. Within this context, your strategy for physician integration should be a well thought-out plan. A proactive approach will allow your organization time to not only develop strategies but to work with stakeholders (including key independent physicians who are not currently interested in employment) to build support. Rather than reacting to opportunities as they arise, you can be proactive in building a network that addresses your strategic priorities, such as strengthening specific service lines or expanding your service area.
Evolution of Management Expertise
Management requirements rapidly become more sophisticated and demanding as a physician network matures, as shown in the table below. Organizations that fail to support the evolution of their management structure are far more likely to view their physician network investment as a financial black hole than a valuable strategic asset.
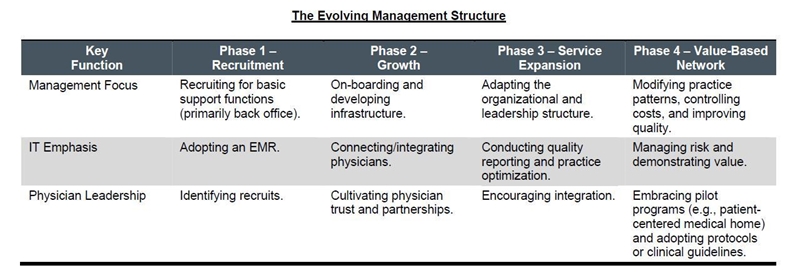
While operating losses can be expected, there are three factors that are essential to financial success:
- Expertise in physician practice management and medical group operations.
- You cannot place a hospital manager, even one with considerable ambulatory experience, in charge of a growing physician network and expect good results. Respect the fact that specific expertise is required, and find an experienced medical practice executive to direct your efforts.
- Physician leadership.
- If your strategy includes partnership with physicians, your management and governance must reflect this commitment. Physicians with potential should be nurtured as managers/administrators and placed in decision-making roles in the physician network, in the hospital, and at the system level.
- Physician commitment to system-wide goals.
- Too often, hospitals employ physicians and then attempt to minimize any behavior or performance expectations in order to be seen as “physician-friendly.” The reality is that providers in an integrated network must be committed to success of the network and compliant with system policies. Improvement in quality and reductions in cost will not occur unless physician behavior changes. If a physician balks at becoming part of a clinical team, he/she may not be an appropriate addition to the employed physician network.
Creating a successful physician network is both a strategic endeavor and a management imperative. While careful planning and precise execution will take more time, energy, and resources, the long-term benefits are worth the near-term struggles.

