
In an effort to address growing national public health risks and concerns regarding COVID-19, Congress passed an $8.3 billion emergency funding package on March 6, 2020, that was signed by President Trump. As part of that package, $500 million is earmarked for expanded Medicare reimbursement of telehealth services. Specifically, it waives the rural geographic location restrictions when an emergency has been declared.
Additionally, dozens of commercial payers have pledged to eliminate copays and deductibles for COVID-19 screening and testing, including via telehealth services. Although patients and providers should check with their contracted payers, we anticipate the list of payers agreeing to cover the costs of COVID-19 screening and testing to grow.

For more information for providers on the COVID-19 emergency declaration, please see this recent fact sheet from CMS.
Regardless of your organization’s current level of IT infrastructure, within five to seven days, your organization can begin providing telehealth services related to COVID-19 screening.
The CDC has created a thoughtful step-by-step checklist for what actions healthcare facilities can take to adequately prepare for COVID-19. In addition to CDC guidelines, health systems should consider the following project plan and steps to rapidly implement a telehealth screening program:

The Call to Action
The CDC has advised healthcare facilities to explore alternatives to face-to-face screenings for the new coronavirus. Given the ease of transmission and the delayed onset of symptoms for COVID-19, healthcare providers are doing as much as possible to keep patients out of clinics and hospitals for unnecessary visits. A primary way to avoid person-to-person contact is through the utilization of telehealth technologies.
How Telehealth Can Help Screen for COVID-19 NOW
Telehealth technologies—phone calls, video calls, chats—enable remote evaluation for COVID-19, as advised by the CDC. The use of telehealth has the potential to:
- Keep people separated, reduce the number of patients coming to the ED, and avoid crowding clinic waiting rooms.
- Prevent unnecessary exposure to germs for patients requiring treatment for other conditions at healthcare facilities and for healthcare providers.
- Allow providers who are under quarantine (related to travel restrictions or possible exposure to the virus) to see patients virtually.
Certainly, there are limitations in addressing COVID-19 via telehealth. Clinicians don’t have the ability to listen to a patient’s lungs without specialized equipment, and a final diagnosis requires a lab test. However, a phone or video call allows patients to receive guidance on whether they need to be seen or tested for the virus.
In addition to screening, telehealth platforms are also a recommended method for monitoring mildly sick COVID-19 patients at home. If appropriate, providers can treat patients remotely—either for COVID-19 to prevent the spread of the virus, or for at-risk patients who shouldn’t be exposed unnecessarily to the virus in a healthcare facility.
Legislative Support and Current State of Reimbursement for COVID-19 Telehealth Screenings
Despite significant adoption of telehealth services by healthcare providers, reimbursement for telehealth visits is not yet an industry standard. CMS has created significant Medicare reimbursement limitations for any telehealth services due to concerns that telehealth services do not decrease overall care utilization or total cost of care. Traditionally, Medicare reimbursement for telehealth services has been limited based on the originating site of care location and to a specific type of provider facility meant to target rural populations.
Health System Role to Facilitate COVID-19 Screening via Telehealth
CMS-published guidelines on addressing COVID-19 include screening staff and visitors about recent travel and determining whether patients need to be triaged to infection control, local public health authorities, hospitals, or self-quarantine. This screening can be conducted via telehealth.
In order to safely and effectively use telehealth technology to screen and triage individuals, a workflow like the process below needs to be implemented.
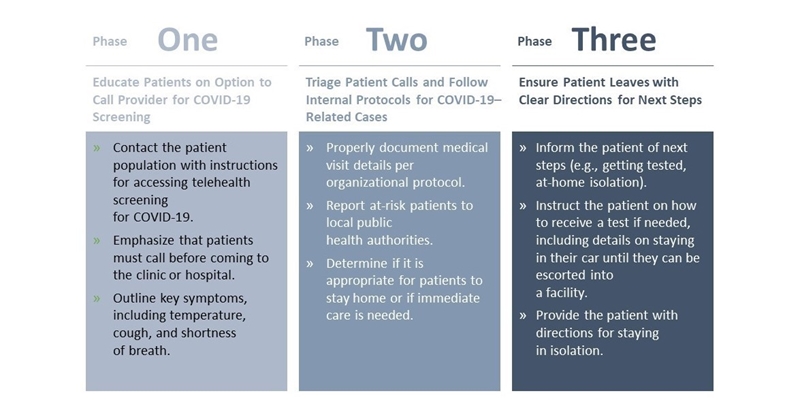
A key component of the successful use of telehealth platforms is the preparedness and integration of a care team supporting the screening providers. It is critical that the support team is trained on how to connect with the local public health authority and follow the local guidelines for procuring and administering tests.
Act Quickly
Time is not currently on our side. Expediency is as important as thoroughness for your COVID-19 telehealth screening plan. It is reasonable to make some of these established plans or protocols temporary and adjustable until full clinical and organizational leadership has had adequate time to review, and to allow for some malleability based on the state of the COVID-19 outbreak in your community. System leadership teams in most metropolitan areas need to be nimble enough to establish their COVID-19 telehealth screening plan in five to seven days if possible, even if some elements of the protocols aren’t fully codified or executed immediately at launch.
We are experiencing an unprecedented challenge to our modern healthcare system. In order to mitigate the spread of this pandemic while simultaneously providing screening and treatment procedures for any patients who may be affected, health systems would be wise to move quickly and develop a comprehensive COVID-19 telehealth strategy.

