
Increasing pressure to improve the value of healthcare has led to innovative models of care delivery such as the Patient-Centered Medical Home (PCMH). This structure emphasizes comprehensive, coordinated, and integrated patient-centered care that aims to improve health outcomes. At the same time, the PCMH model encourages greater efficiency, resulting in reduced waste and lower costs.
However, simply implementing a PCMH is only the first step in a transformative process. This article examines the three phases of the transformation process – implementation, evolution, and integration – and how they form the basis of a successful PCMH. Using these three steps as a guide, health systems can move beyond the implementation of their PCMH model and ensure its long-term sustainability.
PCMH: Key Features
The PCMH fundamentally redesigns the way care is delivered. The following are the key components of an effective PCMH model:
- Team-Based Care – Seamless, comprehensive care is provided by a team of physicians, nurses, medical assistants, case managers, pharmacists, social workers, nutritionists, and other healthcare professionals.
- Patient- and Family-Centered Care – Care is patient- and family- centric, as care teams partner with patients and families to understand care needs and make informed decisions.
- Comprehensive Care – The PCMH provides or coordinates access to all services to meet a patient’s care needs. The primary care physician is responsible for managing a patient’s care from start to finish.
- Coordinated Care – A PCMH team coordinates the patient’s full continuum of care (i.e., primary care, specialty care, hospitals, home health care, and community services). The PCMH ensures seamless transitions between different types of care and clear communication among care providers.
- Access to Care – The PCMH model ensures access to care, services, and information as determined by patient population needs. This model provides alternative means of care delivery and communication (e.g., telephone visits, group visits, patient portals, extended hours, urgent care).
- Care Management – Care teams proactively use population health management, wellness promotion, disease management and prevention, and patient engagement and education to manage their patients’ health.
- Health Information Technology (IT) – Important infrastructure is in place to support the PCMH, including electronic medical records, a patient portal, decision support, predictive modeling, electronic prescribing, a patient registry, and reporting capabilities.
- Quality, Safety, and Performance Improvement – Successful PCMHs commit to the highest standards of quality, safety, and performance by engaging in continuous improvement activities and utilizing best practices and standardized processes.
- Payment Reform – Reimbursement is restructured to appropriately recognize the added value provided to patients who are part of a PCMH.
The Three-Phased Approach
Although many health systems are beginning to adopt a PCMH model, they often lack the resources and knowledge to leverage the model for best results. Our three-phased approach provides a framework with which to implement a PCMH, adapt current systems to fit the new model, and integrate clinical services while supporting the model with innovative financial arrangements. By following this approach, organizations have a structured means of transforming the way they deliver patient care.
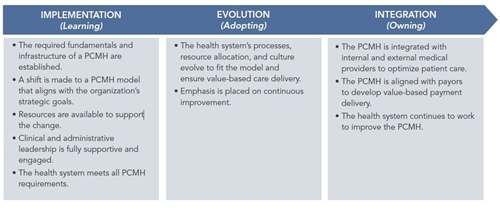
Moving left to right, the graphic below depicts this three-phased approach as a continuum, from implementation to evolution to integration:
Phase I – Implementation
Although the PCMH model has great potential as the future of healthcare delivery, transitioning to a PCMH can be a daunting prospect for any healthcare organization. Many health systems are not yet ready for the transformation: they lack essential change management capabilities, time, or financial capital, or they are not prepared for the substantial cultural or infrastructure changes required.
Those systems that are positioned to move to a PCMH model need to answer some critical strategic questions before they take action at the tactical level:
- How does the model support the health system’s strategic goals and vision?
- How does the health system ensure clinical and financial alignment with the model?
- What infrastructure is required to support the model and other care redesign initiatives over time?
- What are the desired outcomes of the model?
Once the strategic issues are addressed, health systems can move forward with implementation. At its core, the PCMH model will include the aforementioned key components (e.g., patient-centered care, comprehensive and coordinated care, health IT). While the specifics of how to proceed will depend on the capabilities and culture of the organization, a successful implementation will have at its foundation the following elements:
- The commitment and support of clinical and administrative leadership.
- Ongoing clinical engagement.
- Alignment with the health system’s mission, vision, values, and goals.
- Payment methodologies designed to support the delivery of enhanced, value-based care services.
- Staff and leadership with change management skills.
By considering both the strategic and tactical implications of a transition to a PCMH, health systems will be better able to develop a sustainable medical home that provides improved care and services to patients.
Phase II – Evolution
If the implementation phase is about lining up the pieces needed to operationalize the PCMH, the evolution phase is about achieving provider organization and physician buy-in of the PCMH model and having it become a part of the culture and daily processes. Below are some ways that practices can smooth the evolution to a PCMH model and ensure its long-term success.
- Cultural Change – Understand the substantial cultural transformation necessary for PCMH adoption and educate providers on the nontraditional practices of medicine that the model requires.
- Continuous Improvement – Determine the resources and tools necessary to maintain continuous support, development, and improvement of the model.
- Daily Work Flows – Redesign work flows, policies, and procedures to support the model.
- Time – Consider the additional time needed for the transformation and the impact this will have on provider schedules and patient volume.
- Resources – Determine the additional resources needed to support the model.
– Training programs for staff.
– Educational resources for patient engagement.
– Tracking and reporting tools.
– Appropriate staffing levels (e.g., physicians, case managers, nurses, medical assistants, support staff).
– Healthcare IT infrastructure and optimization.
When taken together, these actions help ensure that the introduction of the PCMH model will be as seamless as possible. A smooth transition is beneficial not just for the health system but patients as well – the sooner the PCMH model is fully embraced by providers, the sooner patients will begin to experience improvements in care.
Phase III – Integration
Integration is the natural next step after evolution. In the evolution phase of the continuum, procedures, culture, and behaviors evolve to integrate the PCMH model within the health system. The integration process goes beyond the health system itself to include providers across the continuum of care, such as hospitals, specialty care, and subacute care. At the same time, the PCMH also aligns with payers to take advantage of innovative payment methods that reward value-based care. We examine below how integration can make a positive difference for both clinical care and payment reform.
Clinical Care Integration
While initially the PCMH model addressed primary care medicine, today it focuses on the patient’s total health picture. Toward this goal, the model emphasizes communication and collaboration among all of a patient’s medical providers, including primary and specialty care, hospitals, home health facilities, nursing facilities, and behavioral health.
By coordinating a patient’s comprehensive care needs, the PCMH model integrates the previously fragmented and inefficient healthcare system. The results are threefold:
- Patient care is improved as physicians work together to develop best practices and standardized ways.
- Health systems can better manage patient populations, operate more efficiently, and keep costs down.
- Health systems can position themselves in the competitive healthcare market as high-quality, high-value organizations.
With better integration, health systems and payers are seeing improved clinical and financial outcomes, including:
- Reduced unnecessary ER visits.
- Reduced unnecessary readmission rates.
- Reduced per member per month (PMPM) costs.
- Increased patient satisfaction.
- Reduced patient wait time and improved access to care (i.e., availability of appointments).
- Improved patient outcomes for chronic conditions (e.g., diabetes, cardiovascular disease, hypertension).
The table below presents the clinical and financial improvements already experienced by various PCMH pilots.
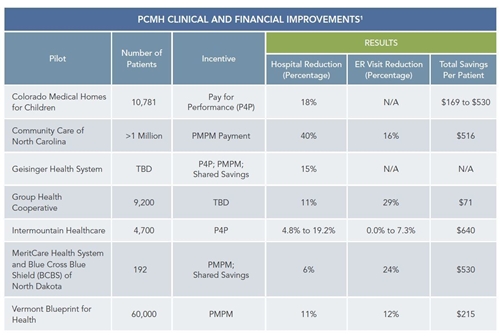
Financial Integration
Transitioning to a PCMH model also means moving from current volume-based to value-based payment methodologies, where the focus is not on the number of procedures performed but patient outcomes. A successful PCMH model will include reimbursement processes that promote high-value care delivery and improved outcomes, while still lowering the total cost of care.
Too often, health systems explore PCMH models and payment delivery options separately, exacerbating the misalignment of clinical and financial initiatives. Healthcare leaders must instead work closely with payers to devise value-based payment methodologies that benefit both parties and support the PCMH’s near- and long-term strategic goals.
When implementing a PCMH model, organizations should consider the following steps to ensure that payment methodologies are supporting value-based care:
- Review current managed care contracts to understand whether they appropriately support value-based care delivery.
- Determine the local, regional, and/or national market trends regarding reimbursement methodologies for a PCMH.
- Determine the organization’s available and needed financial capital to support the model.
- Understand how new payment models will: (1) support the PCMH transformation, (2) affect provider compensation, and (3) help incentivize behavior.
- Begin discussions with payers to design collaborative value-based contracts.
When it comes to implementing a PCMH payment reform strategy, a healthcare organization could include one or a combination of any of the following payment mechanisms:
- Grants.
- Infrastructure support and funding.
- Care management payments.
- P4P.
- Shared savings.
- Global budget or risk-based arrangements.
- Enhanced payments for care services.
It is important to note that, depending on each health system’s needs, the PCMH model requires varied levels of financial investment to fund both the initial implementation and the long-term viability of the model. Government and private payers, such as BCBS, UnitedHealthcare, and Cigna, are experimenting extensively with initial funding and reimbursement methodologies to support the PCMH model.
The Three-Phased Approach in Visual Terms
The graphic below illustrates how the three phases support a successful PCMH.
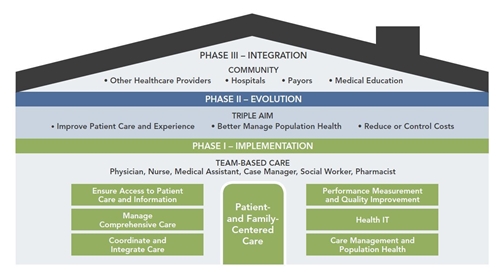
Risks of Inaction
As market forces spur practices toward value-based care delivery, health systems that postpone care redesign will struggle to remain viable in the future. Some potential risks of not moving to a PCMH model include:
- Future incentives and cost-saving opportunities might be unavailable to medical practices that do not have active PCMHs. Examples include:
– Investment in further development of PCMH capabilities and infrastructure.
– Payment for system performance in managing the health of a patient population. - Payers are seeking to partner with providers to undertake population health management initiatives and are using PCMHs as a proxy to identify qualified participants.
- Some payers are designing benefit packages that waive co-payments if patients seek care at a certified PCMH, which could result in decreased patient volume for non-PCMH organizations.
- Inadequate monitoring and coordination of care can result in lost opportunities (e.g., referral leakage).
In short, health systems that fail to adopt the PCMH model risk missed opportunities and lost revenue.
Conclusion
With the PCMH model, health systems can become more efficient, lower costs, improve the way care is delivered, and, most importantly, give patients better experiences and outcomes. In order for a PCMH to be successful and sustainable, it must be done right. This article has proposed a three-phased approach – implementation, evolution, integration – to help health systems transition to a PCMH as smoothly as possible while aligning the interests of patients, providers, payers, and other medical services.
Ultimately, the measure of a PCMH’s success is not how well it functions, but the impact it makes. With an effective PCMH in place, healthcare providers can at last focus on what really matters: delivering value-based care that is truly patient-centered.


