
Cardiologists’ top concern when contemplating employment is their compensation. A close second is the practice governance model and how practice leadership will relate to hospital management and other employed physician practices. Why is this issue of such importance to cardiologists? For a group that has been in private practice, the move to hospital employment represents a substantial loss of autonomy and control. The physicians’ concerns are that the hospital will make fundamental changes to the clinical practice and mandate changes ranging from patient scheduling to compensation allocation. Often, physicians demand to report directly to the hospital CEO, circumvent current employed physician practice governance, and operate in a structure separate from other employed specialists or primary care physicians (PCPs).The right cardiology practice governance model balances the cardiologists’ desire for autonomy and self-management with the hospital and the employed physician practice’s need to coordinate practice operations, create close relationships between all employed practices, drive practice performance, and ensure that the model can be replicated with other practices. Choosing the right model entails making a choice between the level of control to be granted to the group and the need to standardize and centralize practice management and governance within a hospital’s employed physician practice infrastructure. A closely aligned model can also better aid the hospital in preparing for healthcare reform, which includes providing the ability to effectively manage bundled payments and to create an organizational focus on cost and quality. The following chart details the three most common practice governance structures utilized:
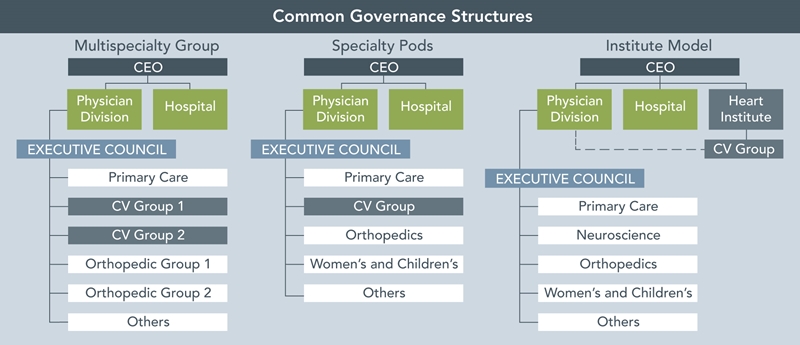
The three models represent potential governance structures, ranging from the multispecialty group, which focuses on creating coordination between all employed practices, to the institute model, which creates a singular focus on employed CV physicians.
- Multispecialty Group – An employed cardiology group(s) is one of many other practices employed and governed by a single entity under a common management structure. This model has the benefit of creating a dedicated infrastructure for the employed physician enterprise and allowing for enhanced collaboration between employed PCPs and specialists. The downfall of this model is that from the cardiologists’ point of view, it does not recognize the unique characteristics of their practice and places them in a structure that is often dominated by PCPs. One concern is that a non-cardiologist will be in charge of making compensation and operations decisions for cardiologists in this model.
- Specialty Pods – All employed cardiology practices, and potentially other CV-related specialty groups, are aligned as a “pod” within the employed physician practice and holistically coordinate governance activities, with representation at the employed physician enterprise level as well. The CV-related physicians have a high degree of autonomy in managing operations within their pod, but also have a presence within the governing body of the larger employed physician enterprise. This model bridges the gap between the cardiologists’ desire for autonomy and the need to utilize a single vehicle for physician employment. It may not go far enough, however, in giving cardiologists a direct line of sight to hospital leadership.
- Institute Model – All employed cardiologists, and again, potentially other CV-related specialists, report directly to the heart institute or CV service line, with a matrixed relationship to the employed physician practice for support services. The model directly aligns cardiologists with the hospital CV service line, creating a powerful tool to develop and enhance CV services and making the physicians partners in the delivery of cardiac care. This can create a model that cannot be duplicated with other specialty areas/service lines, however, and does not fully leverage the value of a large, coordinated physician enterprise.
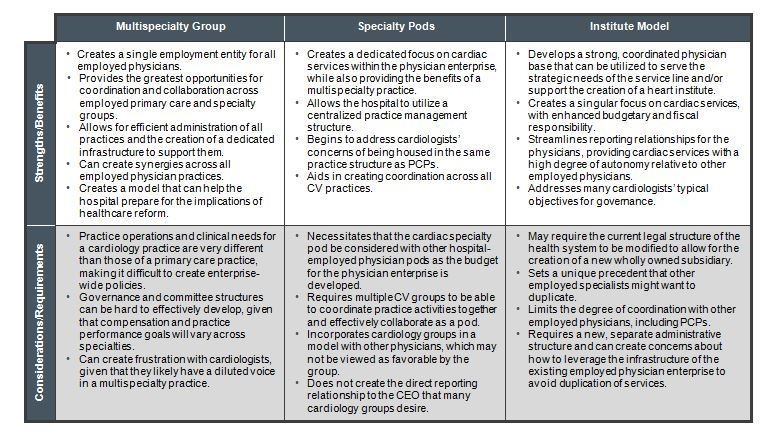
Each of the structures highlighted can be successful if it is chosen to meet the goals of both the physicians and hospital and if it is implemented correctly. The strategic challenge is to ensure that the chosen model is the right fit. The operational challenge is to ensure successful execution. While the institute model might be desirable for leveraging the cardiologists in support of service line development, implications on other service lines must be considered, and the model must have the backing of hospital leadership to be successful. Similarly, if physicians are not supportive of a multispecialty group model, then a structure that is designed to encourage collaboration will not meet its objective. It is critical to understand the objectives of both parties and choose the model that best addresses the goals of each, then tailor the structure to fit the specific context of the organization. When implemented correctly, the right practice governance model can enhance organizational focus, drive coordination of care, and create a culture of accountability. If implemented incorrectly, the governance structure can cause a rift between hospitals and employed cardiologists and fail to meet the potential opportunities generated by physician employment.

