
How Can You Tell If Your Referral System Needs Improvement?
For many health systems, referral leakage may equate to millions of dollars in forgone revenue, as every patient who seeks care elsewhere is a lost revenue opportunity now and potentially into the future. This makes managing referrals to minimize leakage an increasingly important focus area for many organizations. Symptoms of an underperforming referral management system include:
- The inability to identify in-network or aligned providers.
- Insufficient or unclear information for what patient types or conditions a provider treats.
- Limited to no ability to measure referral management team performance or financial outcomes.
- Ineffective prioritization and workload management.
- Increased authorization-related denials and write-offs.
- Reliance on paper-based or manual communication and tracking systems.
- Identification of patient leakage due to complicated, cumbersome, or unclear referral processes.
Diagnosing Your Organization’s Improvement Opportunity
The ability to make significant improvements in referral processing efficiency and patient capture depends on the service’s degree of process standardization and accountability, underlying infrastructure and organization of staff, and technological capabilities.
Process Standardization and Accountability
Inconsistency in the processes and accountabilities between the referring provider’s office and the receiving provider’s office is common. Organizations are often challenged when defining who is responsible for obtaining prior authorizations, locating a specialist with good access who will treat the patient’s condition, gathering relevant medical records, and contacting the patient to schedule the appointment. Organizations with strong referral management programs have developed a consistent and standardized workflow that clearly delineates responsibilities by role. Achieving this level of efficiency requires that operational and clinical leadership collaborate to design and develop policies, procedures, standards, and workflows to support strong referral management practices.
Centralization of Referral Management
Even when standardized workflows have been designed and implemented, it is common for variation to be introduced over time, particularly in decentralized environments where managers have competing priorities and training can be highly varied. Further, clinic-based staff are rarely dedicated to the referral management function, so the work is often deprioritized as other, patient-facing tasks take precedence. To address these challenges, many health systems are adopting a centralized approach to referral management, whereby staff resources are specialized and dedicated to the function. While the implementation effort can be high, it is a relatively low-cost option that can produce tremendous financial and patient-experience benefits.
Technology Systems and Capabilities
Despite having a thoughtful and disciplined approach to monitoring and managing referrals, technology systems are often unable to facilitate best practice workflows or deliver the performance data necessary to effectively manage the end-to-end process. Therefore, manual processes have become commonplace to track authorization status; monitor scheduled appointments; and calculate referral conversion rates, staff productivity, and downstream revenue. Furthermore, the inability to share information electronically among providers necessitates increased use of paper-based and faxing processes. Without the proper supporting technologies, there is increased processing effort and workload, risk of lost or inaccurate data, and, most importantly, the potential to delay patient care. The technological capabilities needed to support a best practice referral management team are described in figure 1 below.
Referral Management

This quiz provides a tool to ascertain the level of improvement potential based on your current-state referral management approach and the three areas of opportunity outlined above.
Future-State Goals
Once the level of performance and degree of opportunity is understood, a roadmap containing the following transition elements is recommended:
- From unclear, disparate processes to ones that are clear and standardized
- From a decentralized referral management function to a centralized one
- From an infrastructure relying on using mixed systems (including paper) to a single technological platform capable of supporting best practice referral management
Measuring Success
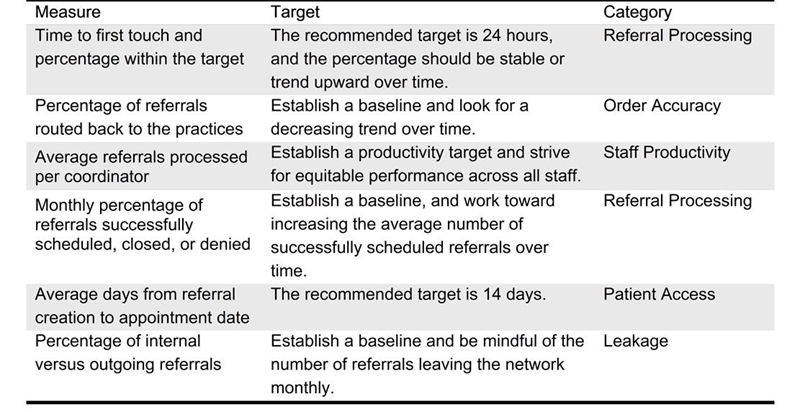
Though many different metrics can be used to track your organization’s journey toward excellence, we recommend those set forth in table 1 to understand your organization’s baseline opportunity and progress.
A Worthwhile Investment in Your Organization’s Future
Investing time and effort in your organization’s referral management requires buy-in and support from multiple stakeholders, including physicians, IT, administrative leaders, project support staff, and your referral coordinators. However, a focused referral management effort, specifically one that is centralized, has the potential to maximize network utilization and revenue collection through dedicated resources, standardized processes, and technology-enabled workflows. Most importantly, improved referral management ensures more patients receive their recommended care in network and in a timely manner.
Take the referral management quiz to ascertain the level of improvement potential based on your current-state referral management approach.

