
Cancer care is perhaps the most dynamic field of medicine. Given the intense focus on improving the myriad of treatment options a cancer program offers, innovation is moving at a whirlwind pace. At the same time, cancer programs are not immune from the macro trends impacting the healthcare industry—specifically, the continued reductions in reimbursement and the expectations for improved clinical outcomes. Generally, the forces transforming the cancer marketplace may be organized into two pillars: here-and-now issues and next-level issues.
Here-and-now issues include:
- Balancing reimbursement pressures and rising costs.
- Redefining access to compete with the rise of consumerism in cancer care.
Next-level issues include:
- Keeping pace with innovation and evolving cancer medicine.
- Preparing for a value-based future.
The confluence of multiple transformational pressures on the cancer care industry not only heightens the importance of strategic planning (so organizations are well prepared to respond to these changes) but also increases the complexity of planning. In a recent planning guide, ECG experts shed light on some potential strategies that organizations may pursue to address these specific challenges. And throughout the rest of this article, we explore a planning framework that may be used to drive successful, tailored, and implementable strategies for contemporary cancer centers.
Only a few years ago, health systems routinely considered long-range strategic planning to reflect a 10- or even 15-year time horizon. Today, most organizations consider three to five years to be long-term planning, given the pace of change in the industry and the level of disruption. Therefore, if you have not developed a strategic plan for your program in the last three years, this is a good time to consider refreshing the existing plan. And if you do not have a strategic plan, you should begin working on one now.
One important note: before commencing your strategic planning, it is critical to first identify and assemble a cross section of key stakeholders to participate. Typically, the most successful planning processes include key physician leaders from across the organization, as well as administrative leadership. The involvement of physician leaders early on is important to build support for both the plan and the change management that will likely be required.
Framework
As Michael Porter wrote: “The essence of strategy is choosing what not to do.” In an era of infinite challenges and finite resources, an organization must employ a very rigorous approach to strategic planning to ensure that financial resources are optimally deployed. Many organizations find value in bringing structure to their planning process by adopting a planning rubric. Commonly, entities use a four-part planning framework that progresses from defining the organization’s purpose to identifying supporting goals and strategies and finally to articulating specific tactics.
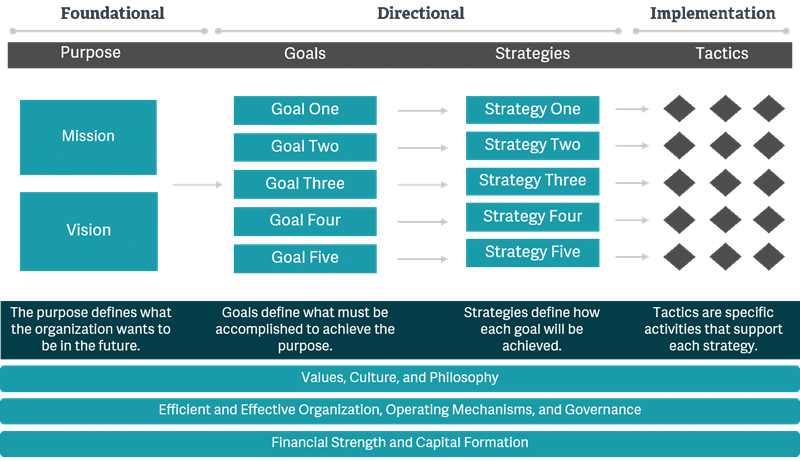
Confounding this process, however, is the fact that cancer programs are really a portfolio of site-specific programs (e.g., breast, prostate, lung). Some may ask, “Do we apply the planning framework at the portfolio level or at the individual program level?” This is an excellent question. In reality, the framework, and much of the content that follows, could be applied at either level. However, in most instances, a hybrid approach is best—developing purpose statements and goals at the portfolio level and developing strategies and tactics at the site-specific program level.
Before launching into a detailed planning process, it is important for an organization to first understand its current performance and critically analyze its challenges and opportunities. As outlined below, following this framework will provide organizations with a blueprint to systematically progress from identifying key considerations and aspirations to creating implementable solutions.
Foundational
The first phase of the planning process involves defining key foundational elements unique to the organization and its aspirations. The mission and vision play an important role in charting a long-term course for the organization and provide a foundation upon which all future decisions will be made.
- Mission: What is the purpose of our organization, why are we in business, and what is our “true north”?
- Vision: What do we aspire to accomplish in the midterm (e.g., 3 to 10 years)?
When establishing organizational foundational elements, key questions to consider include:
- What is most important to the organization?
- How do we define success for the organization, and how will we know when we achieve it?
- How will our organization be differentiated from others that provide similar services?
- Why should future employees or patients be attracted to our organization?
Directional
Following the development of foundational elements, the framework next focuses on directional elements: goals and strategies. These provide increasing levels of granularity to the strategic plan and begin to shape the roadmap for the organization. The goals articulate what the organization will achieve to realize its vision, and the strategies describe how it will pursue these goals.
Goals
Goals define the specific accomplishments that are needed. These include actionable targets such as, for example, establishing a breast program, increasing market share for a colorectal tumor group, or developing an in-house radiation oncology program. Goals should be “SMART”—specific, measurable, attainable, relevant, and timely. The more specific a goal, the more valuable it will be for the planning process; for instance, “achieve a 15% accrual rate for clinical research studies by 2023” is more actionable than “improve research accrual rates.” The number of goals selected should be manageable—three to five are a reasonable target.
Strategies
Strategies should be developed in line with each goal. Choose three to five that articulate the activities that will enable fulfillment of the goals. For instance, for a clinical research goal, the organization might identify a strategy to develop the requisite support infrastructure to enable a high-performing research enterprise. More specifically, the strategies should also identify the site-specific programs that will be enhanced through subsequent planning efforts.
Implementation
The implementation stage involves determining specific tactics to execute the strategies; these should be precisely defined actions. Using the example from above, a tactic to enable development of the requisite research support infrastructure might include hiring a research coordinator during the next fiscal year.
Key Strategic Factors for Oncology Programs
When developing a strategic plan for an oncology organization, there are many topical areas that should be assessed and, as necessary, addressed in the development of strategies and tactics. These include:
- Physician leadership and expertise.
- Quality improvement.
- Research efforts.
- Supportive care resources.
- Screening, education, and prevention.
- Diagnosis capabilities.
- Treatment resources.
- Facilities and technology.
Because these factors will shape the development of strategies and tactics for the program, they should be developed at the site-specific program level. However, before beginning such detailed work, the organization should determine the site-specific programs to focus on, so that detailed planning is not required for all of them.
For each of these topical areas, cancer program leadership should consider what capabilities the program currently has, how they compare to competitors or other leading programs, and how developments in these areas impact the strategies and tactics. Additional information regarding the eight topical areas is presented in the following figure:
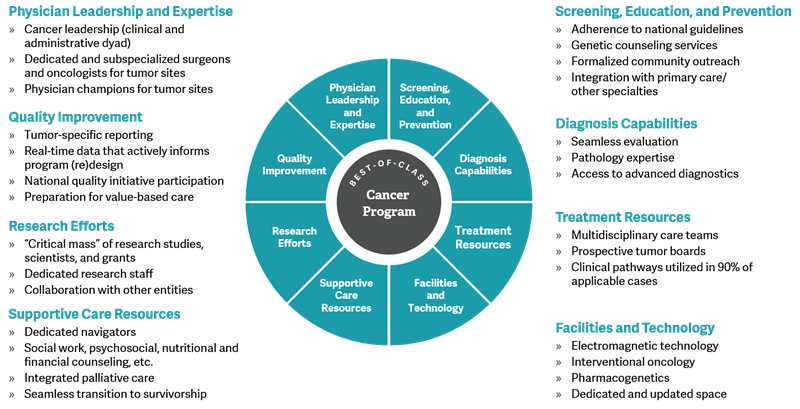
Growth Strategies
For many programs today, realizing larger strategic aspirations requires program growth—whether for achieving scale or generating financial performance to support key investments. Most growth initiatives may be organized into one of two categories: growth in place and regional expansion.
Growth in Place
Growth in place focuses on improving market share within an established service area. As mentioned, the detailed planning (strategies and tactics) should be developed by site-specific program for those programs that have been identified for development/enhancement. Strategies commonly adopted for a growth-in-place framework fall into six categories:
- Physicians: Target recruitment of specific capabilities to augment the program, often from a leadership, clinical, and/or research perspective.
- Staff and Support: Identify specific needs to enable greater differentiation of the program, which may include administrative leadership, patient support services, navigators, or other personnel.
- Technology and Facility: Make specific investments to either modernize the program (keep up with community standards) or to differentiate it from competitors, either from a clinical or aesthetic perspective.
- Program Organization: Develop constructs to better organize and manage the program while at the same time improving physician engagement.
- Financial Support: Identify and obtain additional funding (from within or outside the program) to enable other strategies.
- Coordination: Improve communication and coordination both among care team members and between the care team and patients (e.g., secure messaging, better navigation processes, multidisciplinary clinics or conferences).
When selecting strategies to support a growth-in-place approach, it is important to consider not only the competitive landscape but also the patient perspective. As demonstrated by a recent patient survey and illustrated in the figure below, specialized clinical capabilities and differentiated outcomes matter most to patients when selecting a cancer services provider. Therefore, subspecialty provider recruitment often tops the list of key strategies to be employed.
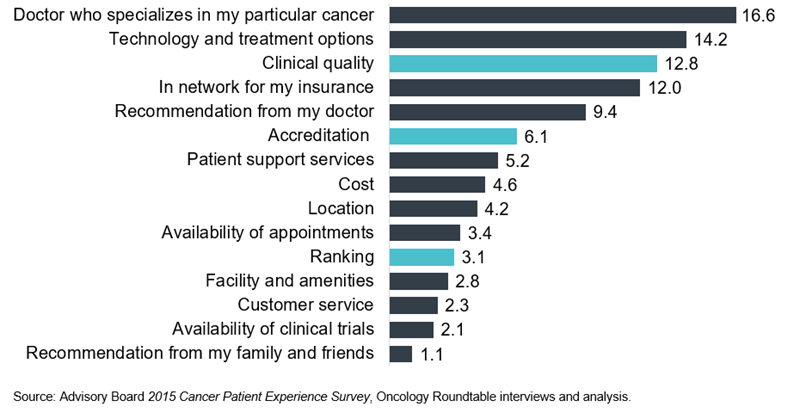
It is also important to keep in mind that growth strategies do not always require expansion of physical assets. In fact, the organization can often unlock additional capacity through process improvements (e.g., scheduling, staffing) using existing assets. These topics will be explored in greater depth in a future post.
Regional Expansion
Alternatively, regional expansion moves beyond growth in place and focuses on enlarging the geographic area that is served. Regional expansion is typically considered once an organization has attained high levels of performance in its existing service area and clinical portfolio. When contemplating regional expansion, there are three factors that must be addressed:
1. Decide where to expand.
- Determine the desired features for future markets.
- Evaluate and prioritize potential markets.
2. Establish the number of new sites desired.
- Determine the size of new locations (e.g., scope of clinical offerings, square footage).
- Establish options for new sites based on available resources (e.g., capital, personnel).
3. Define a development strategy.
- Determine strategies to successfully enter into a new market.
- Build capability internally.
- Purchase existing capability.
- Closely align independent groups.
How This Applies to Your Organization
There is no one-size-fits-all approach to strategic planning or growth. Every entity faces unique market conditions determined by the resources both within and outside the organization. The framework described in this article will allow you to tailor a strategy to the specific circumstances your organization faces.
In our experience with hundreds of strategic plans of organizations throughout the US, we have learned that there is often as much value in the planning process as there is in the outcome. The planning process is a critical part of organizational change management and is imperative to building consensus among a large and diverse group of stakeholders. Moreover, given the pace of change in cancer care today, the highest-performing organizations will develop processes and leadership frameworks that allow them to continually reassess their strategic position, making minor updates to their plan frequently rather than major updates every few years. Such an approach to cancer services strategic planning ensures that organizations optimize the use of human and capital resources, as well as keep up to date on innovations in oncology care. This approach will also help the organization to pivot more effectively—from focusing on one site-specific program to cultivating another and/or identifying necessary operational improvements to support strategic efforts.

