
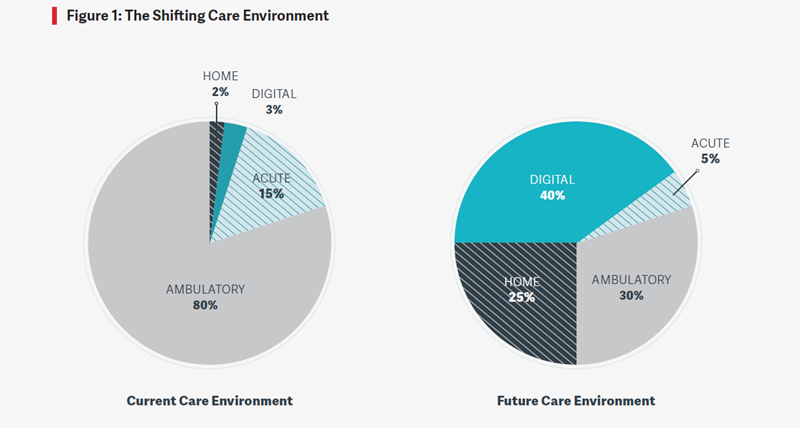
Healthcare facility managers are often responsible for executing strategic plans and allocating capital dollars to facility improvement projects, but they are not always involved in the strategic planning process itself. As the healthcare environment continues to undergo dramatic changes, there will be a substantial impact on the physical assets used to deliver care (see figure 1). Organizations that engage facility managers in the strategic planning process will be able to utilize their teams fully and remain competitive. To be effective, facility managers need to understand the impact of these care delivery shifts and prepare for them, developing the tactics essential to executing strategies for success in the future.
Decreasing Acute Care Will Drive a Greater Need to Use Resources Efficiently
Aa patients with more basic conditions are increasingly treated outside of the hospital setting, conventional hospitals will be used for a more limited, acute patient load where each patient requires more resources than before. This shift is expected to result in a 10% decrease in acute care delivery, moving from 15% to 5% in the future.
How to Prepare: As patient volumes in the hospital decline, so too will traditional hospital-based revenue. But as all hospital facility operators know, hospital buildings aren’t getting any younger, and compliance with code requirements isn’t getting any easier. With fewer dollars to spend on fixed hospital assets and higher standards to meet, facility managers will need to determine which assets need to be upgraded, which should continue operation with maintenance, which should be repurposed, and which should be phased out. A facility condition assessment is the first step in this process, and linking these conditions to the strategic planning process—and doing so regularly—will help ensure that resources are prioritized for the highest and best use of each asset in the future.
A Decrease in Ambulatory Care Will Increase the Need for Interdisciplinary Teams
An essential element in the transformation of care delivery is the move to more patient-centric, community-based care. In order to compete in this new environment, healthcare systems will attempt to provide care either in the home setting or as close to home as possible. In the case of ambulatory care, this strategy will require more locations, even as the percentage of care delivered in the ambulatory setting declines from 80% of care delivery to 30%. Ambulatory care sites of the future will need to house multiple services and clinical specialties and support an array of physicians and specialists on any given day.
How to Prepare: Developing space operating plans that emphasize flexibility and adaptability will be a critical component of a successful facility operator’s role. Maintaining this operating model will require a workforce that is trained on multiple systems; can work independently; and has the right IT resources to effectively manage a diverse, geographically dispersed portfolio. Investing in resources and training today will pay dividends in the future.
The Shift to Home Care Will Redefine the Role of Facility Operators
Home-based healthcare delivery is expected to increase from 2% to 25% in the future. This shift means that more healthcare equipment will be integrated into the home setting. To gain an edge, healthcare systems can look to facility operators, IT departments, or biomedical engineering staff to help determine how to best deliver the necessary supplies and how to safely monitor patients once the equipment is in the home.
How to Prepare: Delivering healthcare in the home will require nimble, multidisciplinary teams to manage patients and to make certain that effective communication is supported between the home and the hospital, guaranteeing that patients have what they need when they need it. Facility teams will integrate with care coordinators and patient navigators to allow the seamless transition of patients to the home setting. The role of facility experts on these teams will be to ensure that implementable strategies are selected to efficiently and cost-effectively deliver specialized care to patients at home.
The Increasing Prevalence of Digital Visits Will Impact Network Infrastructure and Facility Deployment
Although digital care delivery is projected to increase by 37%, from 3% to 40%, the need for fewer beds and in-hospital care spaces does not necessarily mean less space will be needed for providers or equipment. Facility operators will be responsible for providing and maintaining the infrastructure for site-to-site and site-to-home communication.
How to Prepare: The transition to digital healthcare will require added medical equipment as well as computers and technology infrastructure. Partnering with community providers (i.e., pharmacies) to build a comprehensive digital health strategy and ensuring that patients who are not tech savvy are able to access the same level of care are two key challenges to enabling a successful digital strategy. In addition, facility operators will be required to enable this strategy with the right back-end support, such as server rooms and other traditional IT equipment. Training or hiring staff who are able to manage the full spectrum of technology equipment will be critical to facilitating this type of digital strategy, and taking part in the planning process will help ensure that pragmatic, implementable systems are selected and integrated as health systems move to make this shift to digital care.
Preparing for the Future
As healthcare systems move into the future, an essential component to their success will be ensuring that facilities are positioned to support this shift and that the facility operators are engaged early and often in the planning process. By doing so, health systems will improve strategic planning, gain a better understanding of the flexibility of current assets, and ensure the smooth implementation of new, groundbreaking models of care.
Understand where healthcare is heading.
Learn more about the shifting care delivery environment and the transformational drivers of the health system of the future.

