Overview

Artificial intelligence (AI) presents compelling implications for healthcare, and the opportunities inherent in an organization’s ability to use big data, complex decision trees, and machine learning align well to assist with the current challenges within the industry. The capabilities of AI and other technology-based tools to improve data accuracy and process efficiency and support overall financial improvement for the revenue cycle present compelling cases for organizational investment.
The estimated impact attributed to AI is more than $150 billion in clinical and operational savings worldwide by the year 2022, according to a recent Frost & Sullivan study. For revenue cycle leaders, there are many opportunities to harness this technology to improve performance. Just as clinical workflows should engage resources at the top of their license, taking advantage of AI is a way to ensure you are getting the maximum benefit from your staffing, technology, and organizational management investments. The ability to take large portions of data and identify predictive algorithms, determine repetitive tasks, validate financial results, or uncover codependencies are all examples of where AI can be implemented to enhance your revenue cycle’s performance.
The Role of AI in Revenue Cycle: Opportunities to Consider
AI has implications across the revenue cycle, from discrete processes to holistic data analyses across the continuum. Opportunities will continue to expand as greater complexity is inherently introduced through expanding clinical protocols and increasingly complex payer contracts, as well as the availability and warehousing of comprehensive data sets.
The following figure shows some of the existing functionalities of AI within the healthcare revenue cycle:
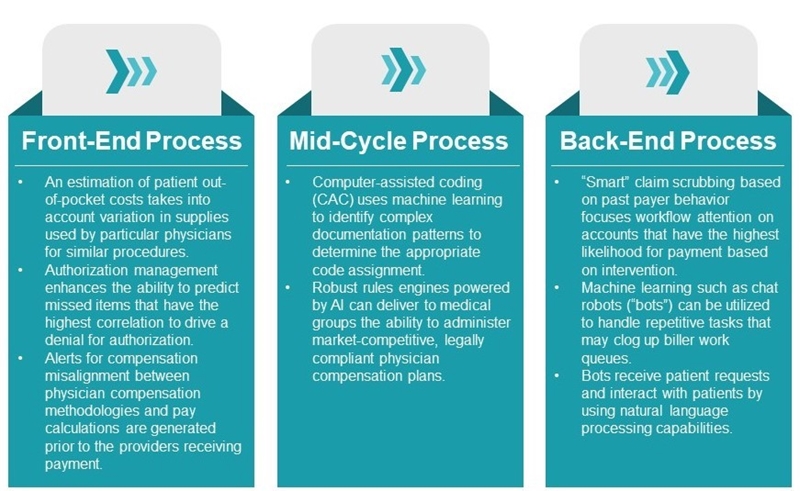
In addition, cross-functional processes are listed below.
- Exceptions-Based Reporting: Details statistically significant departures from the norm so the organization can focus on opportunities for improvement
- Real-Time Quality Assurance: Strives to ensure data is as clean as possible for use downstream in the revenue cycle
- Physician Compensation: Effectively tracks and measures physician compensation plans against organizational goals
- Denial Management: Provides the ability to uncover cross-functional or codependent trends and, in doing so, helps lead to root cause identification and targeted action plans specific to payer, provider, or other specific process gaps
- Data Normalization: Normalizes content across hundreds of different commercial and government payers and product types to create consistency
- Data Mining: Analyzes data to derive significant insights based on patient attributes to determine appropriate actions (e.g., gender, medical history, income) or expectations
- Process Automation: Utilizes software designed to interact with the EHR’s user interfaces to automate repetitive, time-consuming manual tasks
Understanding the Business Case for AI Within Your Organization
The return on investment (ROI) for AI technologies is based on an organization’s ability to apply them to core functions. Asking the following questions about your current business environment will help determine whether taking the next step makes financial sense for your organization:
Will this complement our current approach?
- Elimination of manual data entry
- Enhanced claim scrubbing
- Predicting which claims are at the highest risk of being denied
- Automated confirmation/reverification of insurance
- Predictive screening for Medicaid and charity care
- Propensity to pay
- Initial action steps to address no response from payer after claim submission
- Denial prevention
Does this reduce or replace repetitive tasks that are currently performed manually?
- Automatic adjustment based on standard denial scenarios
- Response to request for information
- Account status check (through clearinghouse or direct screen scrape from payer)
- Scheduling appointments or providing answers to patient questions via bots
Does this unlock a potential revenue stream?
- Enhanced contract management to address carve-outs, outliers, or other value-based payments
- Insurance discovery for existing self-pay accounts
- Identification of secondary insurance
- Identification of complex denial root cause scenarios
Benefits Realization and the Future of AI: the “Magic 8 Ball”
As with any technology implementation, the focus should be on benefits realization. Key metrics should be developed and monitored prior to, during, and after implementation to determine the overall impact. Using the Magic 8 Ball for our examples, we provide a framework for evaluating if an AI functionality is right for your organization.
“You may rely on it.” Or “Signs point to yes.”
Consider options that complement existing processes (e.g., CAC) or eliminate repetitive tasks (e.g., automated claim status reporting); these that will certainly provide value, reduce dependence on scarce resources, and allow your organization to make the best use of valuable staff hours. In many cases, by implementing technology that streamlines workflows, your organization will be able to achieve higher overall productivity and accomplish more with existing resources.
“Reply hazy, try again” or “Cannot predict now.”
AI solutions that focus on unlocking revenue streams have the potential to enhance an organization’s bottom line. The caveat is that they often require the ability to harness big data and can be situation dependent. For organizations that have a strong data warehouse and modern technology infrastructure, the effort spent working with the data is worth the time. This is particularly relevant when many complex or risk-based payer contracts are in place.
If AI offerings are not implemented appropriately or without consideration for ongoing management and performance monitoring, your organization may not enjoy their benefits. A focus should be placed on the technologies with demonstrated business cases based on ROI.
“My sources say no.” or “Outlook not so good.”
It has been considered, but complete automation of the revenue cycle is likely not a near-term reality. Although there are more use cases and great opportunities to target specific tasks, this market is still relatively immature and undefined, requiring organizations to proceed with caution.
As AI continues to take on a larger role within healthcare, successful organizations would do well to keep the following key concepts in mind:
- Focus on what you are good at and seek ways to complement it (“good to great!”).
- Acknowledge your challenges and limitations by determining ways to optimize technology and support to unlock potential avenues for improvement.

