
Price transparency is not a new concept for the healthcare provider market. There has been a year-over-year increase in consumer out-of-pocket cost and recent legislation requiring online access to provider charge master pricing. This is spurring heavy investment from technology and revenue cycle vendors looking to capitalize on closing the knowledge gap for estimating out-of-pocket costs that are specific to an individual’s scheduled services and their respective health plan. Many states now also have transparency websites that compare price and quality for inpatient and outpatient services using all-payer claims databases. This data is great for consumers, as it can be used for shopping and household budgeting. However, these advances in transparency create unique challenges for healthcare providers, and the data available does not always translate into a patient’s out-of-pocket cost, which can be confusing and misleading for consumers.
All Payer Claims Databases (APCDs) for Price Transparency at the State Level
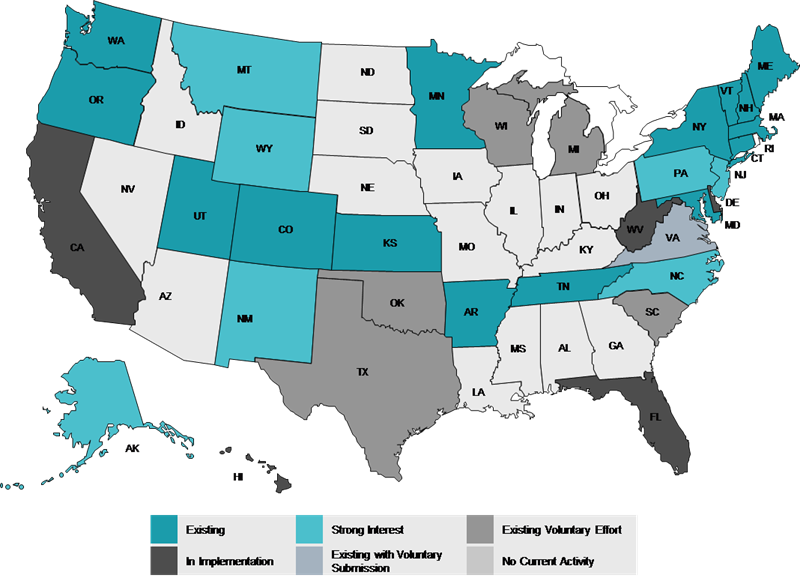
New Era in Definition of Price
From the healthcare provider perspective, there have traditionally been two disparate definitions of price and different domains managing them. First, there is the retail price definition as established in an organization’s charge master file. These are the charge amounts that are debited to a patient encounter in the EHR and translate into gross patient service revenues. Retail prices show up on an itemized bill and are the rates that often make media headlines. The second definition of price is that of the negotiated payment or reimbursement rates from a third-party payer. Whether the payer source is a government or commercial health plan, these prices represent the actual amount of payment a provider organization expects to receive for a given patient encounter; they roughly translate into net patient service revenues.
Though these pricing systems are often managed by different departments within a provider organization, their definitions are widely understood internally. An emerging challenge is that they are not easily understood or communicated to the consumer, who cares about the impact to their out-of-pocket expense, not about the gross charge. The Centers for Medicare & Medicaid Services’ (CMS’s) FY 2019 IPPS final rule requiring hospitals to post charge amounts for all services on their websites in a machine-readable format—along with the aforementioned state-run price comparison sites—is expanding the consumer’s previously singular definition of cost to now include provider definitions of price. These concepts and the related economic and accounting mechanics are so complex that it is unreasonable to expect the consumer to understand them based on a simple shared charge master file. To truly excel in this new era of price transparency and patient financial experience, providers must mitigate confusion and educate their patient populations, going beyond the current CMS requirements to simply post their charge master. Healthcare executives must embrace the continued push for transparency and proactively communicate their organization’s value proposition as it relates to price and quality and provide easily accessible and accurate out-of-pocket expenses for each patient it serves.
Integrated Approach to Pricing
Because rate transparency is increasingly focused on the retail price, regardless of its actual utility to the consumer, under current legislation healthcare providers must take ownership of these established charge amounts and defend them as reasonable to the public. As such, healthcare executives need to answer the following questions:
- How do our retail prices compare with those of competitors?
- For which services are consumers most price sensitive?
- For which services and sites of care can we adjust prices without losing revenue?
Answers to these questions can be found only through comprehensive data analysis that takes into account competitor and internal charge master prices; payer contract rates; payer mix; utilization; and sophisticated “what if” modeling. This data is required to make informed decisions about altering charge amounts, negotiating payer rates, and determining the respective revenue implications of those changes. However, the reality is that net revenue neutral changes made to the charge master’s retail prices are for optics only. Without lowering the organization’s actual reimbursement rates, the effect on the consumer’s out-of-pocket cost is zero. Therefore, this reality creates the impetus for an integrated approach to pricing analytics and decision-making that requires an interdisciplinary team of stakeholder departments, including finance, revenue cycle, patient access, managed care, and strategy.
Where Organizations Should Start
Pricing is a complex discipline and one that requires significant resources to manage appropriately. Further, because price is a major component of patient access and an opportunity to slow the growing costs of healthcare, it is an area on which regulators, employers, payers, and nontraditional providers will continue to focus. If an organization has not conducted a comprehensive pricing review in several years, the place to start is with a benchmarking assessment of both charges and negotiated payer rates compared to those of local market competitors. At a minimum, a review of the most “shoppable” services (e.g., diagnostic radiology, labs, therapies) should be reviewed. Additionally, an assessment of the organization’s technology capabilities should be conducted. This review should include the charge master and payer contract modeling capabilities to analyze the revenue implications of any charge and negotiated rate changes, as well as the ability to accurately provide patients with out-of-pocket estimates for all scheduled visits.
These capabilities are important to a healthcare provider not only because competitors have increasingly developed the intellectual and technological means to perform necessary analyses but also because well-informed pricing is a strategic imperative for the future. Pricing should not be seen as a onetime project or discussed only when payer contract negotiations commence; it should be included in the organization’s annual planning cycle. This means that changes in revenue resulting from the annual pricing review should be reflected in the organization’s integrated strategic and financial plan and operating budgets. For organizations that determine the need to lower prices to remain competitive, a multiyear roadmap should be developed that maintains financial integrity.
Investing in an online price estimator that can accurately calculate patient out-of-pocket expense can also be a marketing advantage for hospitals and medical groups that truly want to show transparency and improve patient financial experience. The most critical aspect to implementing an estimator tool is obtaining quality data and ensuring accuracy in estimated ranges. For example, one problem that has surfaced with these tools is that the estimate may not reflect the full cost of care because of missing professional fees or unanticipated services that were added at the time of service. With quality input and tracking to understand the link between online estimates and actual patient visits, implementing a user-friendly and easily accessible pricing tool could significantly boost hospital volumes, revenues, and patient satisfaction.
Price Transparency as a Strategic Differentiator
Healthcare providers will increasingly compete on price, particularly as new entrants look to take market share for high-margin, mostly commoditized services. Because these nontraditional providers may be either nimble, risk-tolerant startups or well-capitalized Fortune 50 companies, most hospitals and health systems will simply not be able to compete on price alone. As part of their organization’s comprehensive strategic plan, healthcare executives should embrace the push for price transparency and use it as an opportunity to rethink current approaches to access, patient experience, pricing, self-service technologies, and patient-friendly billing. Patients want a seamless healthcare experience customized to their specific situation and needs, and this starts with access to services and accurate pricing information.

