
Businesses that restrict customer or client access to services should not expect to be in business for long. Yet in healthcare, provider organizations have a long history of building barriers to patients obtaining care. There are a litany of ways organizations hinder access: answering telephone calls only during limited, inconvenient hours; failing to fully develop Web-based access points; restricting physician schedules based on what works best for the organization (not its patients); having too many points of contact for seemingly basic tasks, like reaching a nurse; and the list goes on. In the new healthcare environment, health systems and provider groups need to find ways to break down barriers to care – and patient contact centers represent one strategy for doing just that.
Customer service call centers are standard for many industries but less common in healthcare, even among the largest providers. Call centers were once thought to be the antithesis of patient-centeredness, as patients were routinely put on hold for long periods of time, spent more time interacting with voice prompts than live voices, and had to be rerouted to different points of contact for simple questions or requests. Yet today’s patient contact center, when designed and implemented as a true extension of the physician practice environment, creates significant efficiencies for healthcare organizations and contributes to substantial improvements in patient access and satisfaction.
Patient Contact Center Benefits
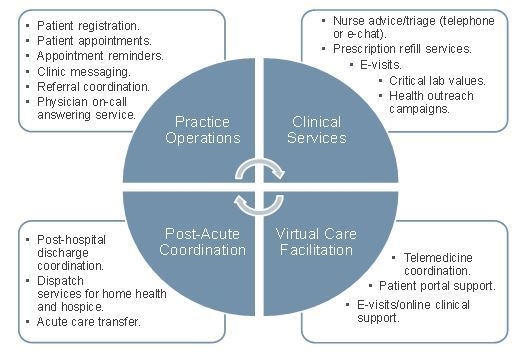
The capabilities of patient contact centers far exceed answering and directing calls. High-functioning contact centers are able to efficiently facilitate both clinical and nonclinical services as well as coordinate care across the system. Examples include referral management, 24 hour nurse advice, e-visit capabilities, and post-hospital discharge outreach.
When designed correctly, a patient contact center can offer significant benefits to patients as well as health systems, such as:
- Providing higher levels of service, in terms of increased speed to answer calls and lower call abandonment rate
- Streamlining multiple-appointment booking across care sites or clinical services
- Allowing practice sites to focus on the clinical provision of care, not administrative processes
- Standardizing operational procedures that tend to be difficult to monitor/change in the individual practice setting (e.g., provider scheduling rules, patient information verification processes)
- Leveraging economies of scale in staffing that cannot be realized at individual locations
- Preventing referral leakage outside of the system/network
- Introducing new access points (e.g., 24-hour services)
Key Questions
Before running to invest in a contact center, however, there are critical questions that physician groups need to ask themselves:
- How complex and variable are current patient scheduling practices?
- To what extent is the organization willing to embrace standardization/centralization, given that the transition to a patient contact center may require:
- Staff relocation or displacement
- Limitations on physician and practice scheduling preferences
- Significant change management efforts
- Do current service levels suggest a need to centralize contact center services to enhance the patient experience? What areas (e.g., scheduling, referrals, nursing) are most critical to address?
- To what degree is the organization’s payer strategy aligned with making additional investments in outreach and population health management activities that may not be in place today?
- Is insourcing contact center services strategically and financially feasible, or can the desired results be achieved through outsourcing to an external partner?
Contact centers are not the right solution for every physician group or health system, but they should be considered within an organization’s overall patient access strategy as part of the move from provider-focused to patient-centric care delivery.
To learn more about patient contact centers, read the full article.

