Generally, we attribute our health status to genetics and lifestyle choices. While these factors, combined with the availability and utilization of healthcare services, do influence our health and well being, we must consider another element that contributes to health status and health outcomes: social determinants of health (SDOH).
The impact of SDOH extends to most aspects of our lives, ranging from the ability to obtain an education to holding a steady job. According to the US Department of Health & Human Services’ Healthy People 2030 initiative, SDOH are “the conditions in the environments where people are born, live, learn, work, play, worship, and age that affect a wid range of health, functioning, and quality-of- life outcomes and risks.”
SDOH DOMAINS THAT DETERMINE HEALTH OUTCOMES
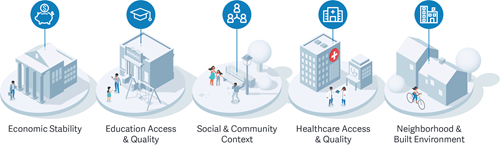
In addition to health outcomes, a key focus of addressing SDOH is achieving better health equity across populations. SDOH factors shed light on why people born a few miles away from one another can experience vast differences in life expectancy—in some cases, differences of up to 25 years.
Addressing health inequities translates to reducing the gap in patients having differences in length of life or number of diseases due to their social position or other associated circumstances. As a result, a population with poor socioeconomic status would potentially no longer be predisposed to adverse health outcomes.
For most healthcare organizations, serving in some capacity to mitigate SDOH is a logical step—it builds on a rich tradition of caring for the community. Healthcare organizations have varying reasons for investing in SDOH. While one reason may be a civic- or mission-based strategy founded on the needs of the community (e.g., helping reduce the area’s unhoused population), another may be an emphasis on helping the community to become healthier (e.g., implementing a nutrition program) with the intent of reducing preventable healthcare utilization. Others might be focused on transportation as a means to aid access to medical appointments, education about self-care, or adherence to medications (e.g., mail order), any of which might lead to better health outcomes.
No matter the organizational motivation, our collective healthcare system has an obligation to improve the outcomes and quality of healthcare for patients. A 2011 study estimated that approximately 900,000 deaths per year were attributable to social factors in the United States. Addressing SDOH would not only provide equitable outcomes for various populations—it could potentially prevent the loss of thousands of lives every year.
In addition, improving SDOH would dramatically reduce overall healthcare spending, as there would be a decrease in hospital readmissions and unnecessary utilization, preventing leakage in revenue and reimbursement.
While much has been written about the importance of healthcare organizations addressing SDOH, this paper provides a framework for how to approach SDOH initiatives.
Get going with SDOH initiatives
Get the guidance you need to identify, prioritize, establish, and measure SDOH initiatives.
This whitepaper was written in partnership with Veronica (Ronnie) Oestreicher, MPH, Principal at CSuite3.

